)
)
)
)
)
)
)
)
)
)
)
)
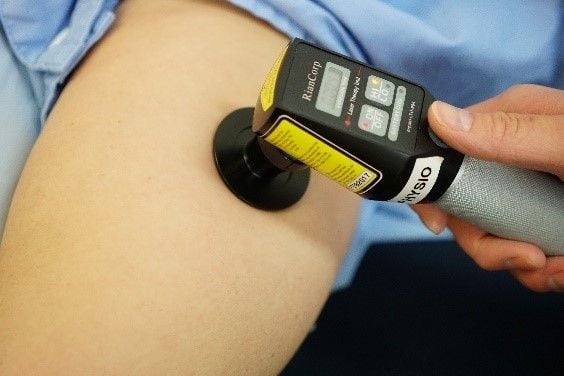)
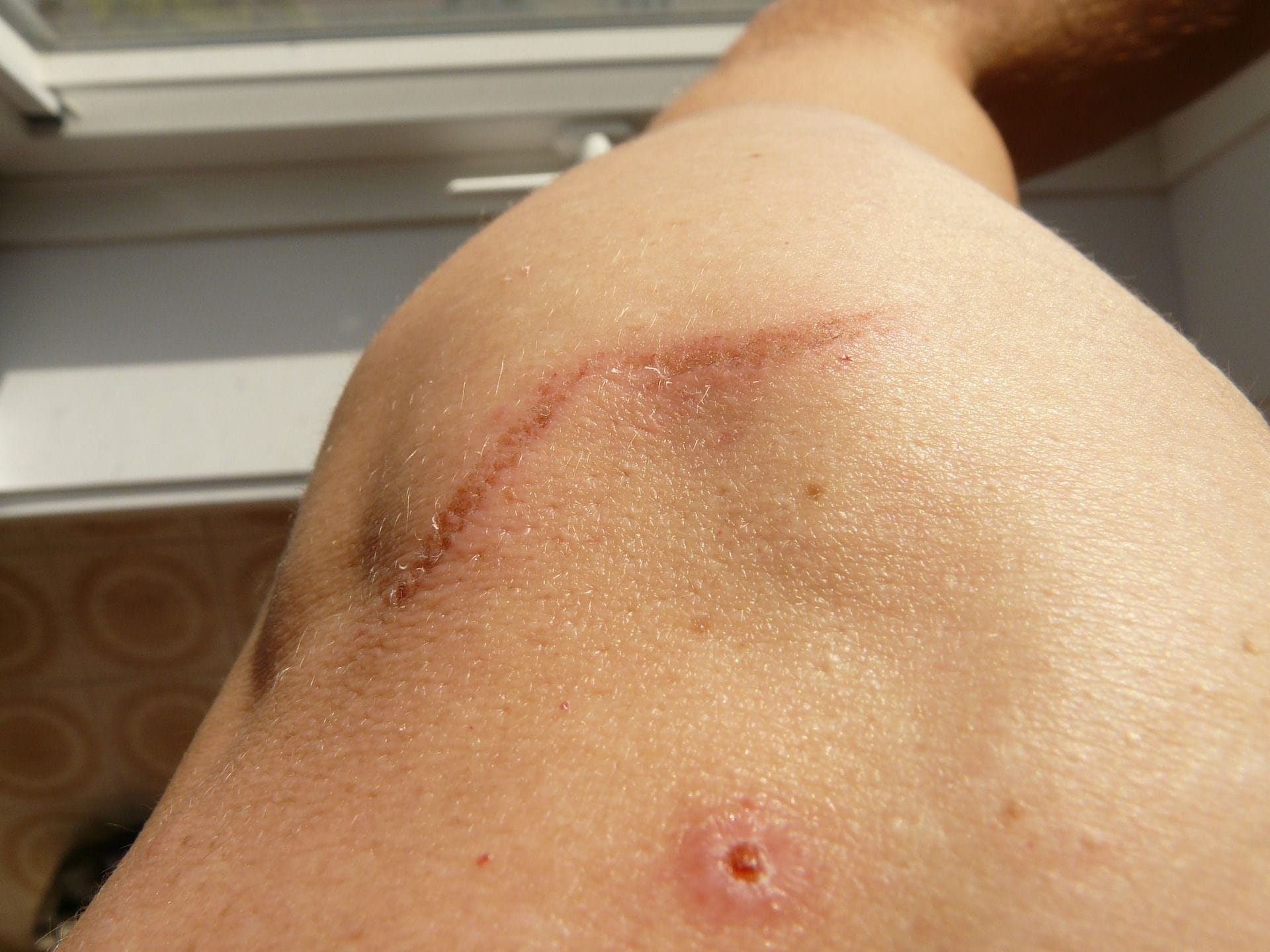
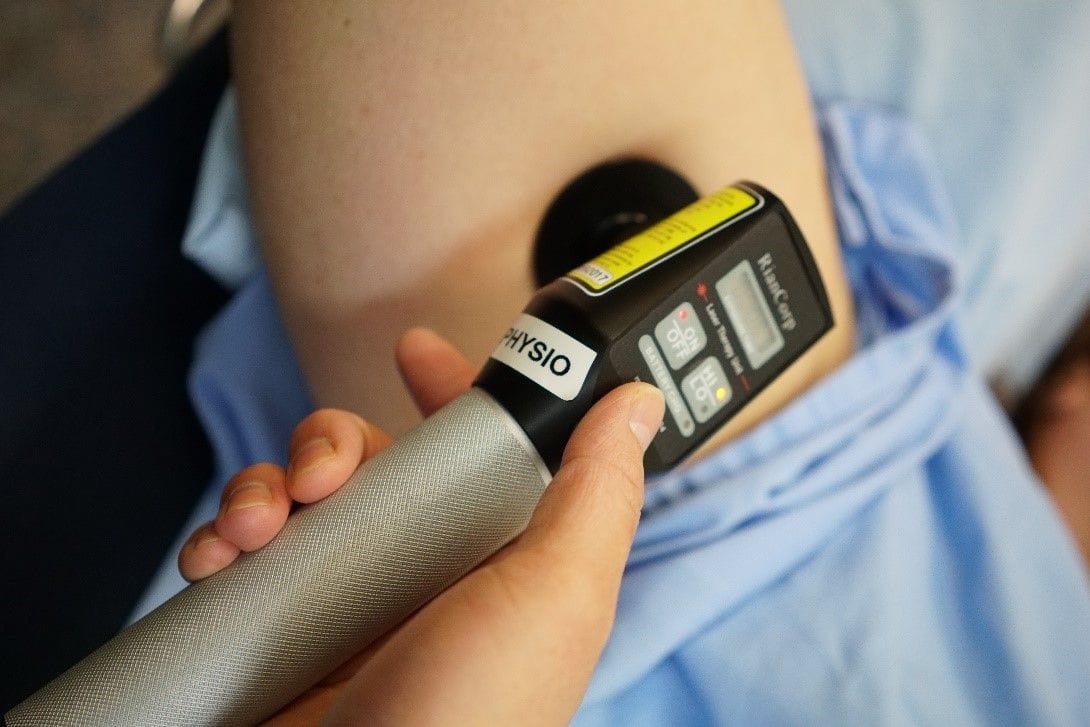
(https://www.riancorp.com/the-product/how-to-use-the-ltu-904)

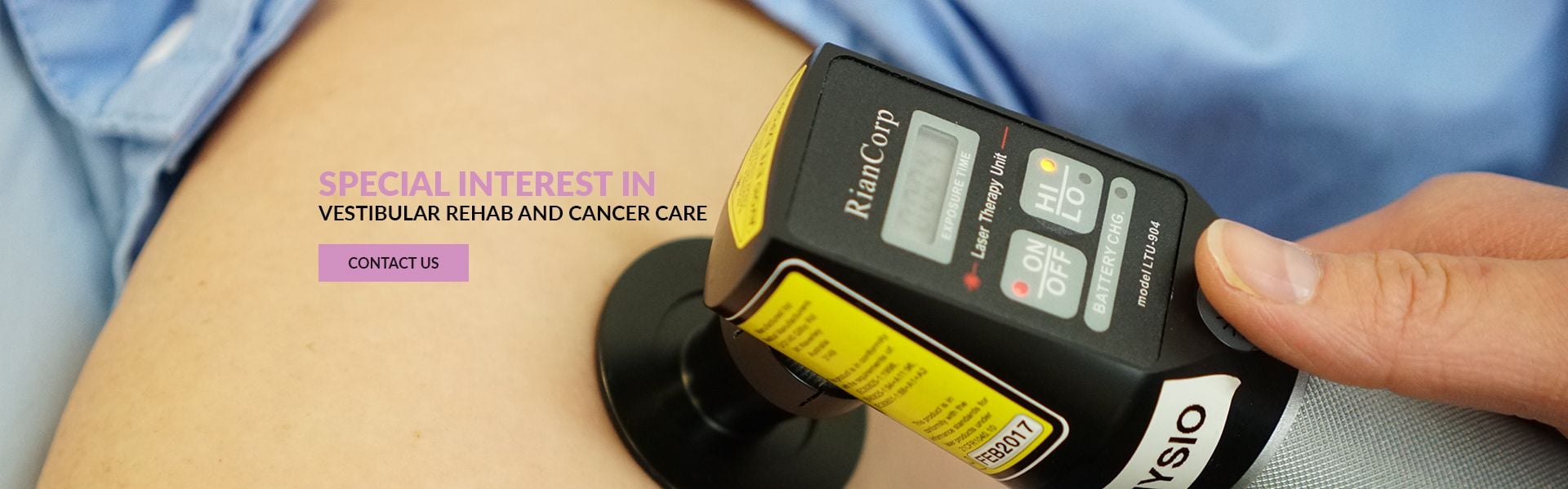
| Tags:LaserMusculoskeletal Conditions |
)
| Posted in:LaserLymphoedemaMassagebreast cancer |
)
| Posted in:VertigoCOVID-19 |
Our physiotherapists are trained to recognise, assess and treat patients that are suffering from vertigo from a vestibular origin such as Benign Paroxysmal Positional Vertigo (BPPV), vestibular neuronitis/labyrinthitis and following acoustic neuroma resection.
read more